
After taking the Pediatric Abusive Head Trauma Quiz, it’s time to reveal the answers and learn more about this serious condition that affects infants and young children. Abusive head trauma, also known as shaken baby syndrome, occurs when a child is violently shaken, causing severe injury to the brain and skull.
Answering the quiz questions correctly is crucial to understanding the signs, symptoms, and consequences of abusive head trauma. By knowing this information, medical professionals, caregivers, and parents can better identify and prevent these cases of child abuse.
One of the key answers to the quiz is that abusive head trauma often results in long-term consequences, including cognitive impairment, developmental delays, and physical disabilities. It is essential to recognize the signs early on to provide immediate medical attention and prevent further damage to the child’s brain.
Overall, taking a quiz on pediatric abusive head trauma is an important step in raising awareness about this critical issue. By understanding the answers and learning more about the condition, we can all work towards preventing these cases of child abuse and ensuring the well-being and safety of our youngest and most vulnerable population.
Pediatric Abusive Head Trauma Quiz Answers

Abusive head trauma (AHT), also known as shaken baby syndrome, is a serious form of child abuse that can result in severe brain injury or even death. It is important for healthcare professionals to be able to recognize the signs and symptoms of AHT in order to provide appropriate care and support to affected children and their families. In this quiz, we will review the answers to common questions about pediatric abusive head trauma.
1. What are the signs and symptoms of pediatric abusive head trauma?
- Extreme irritability or lethargy
- Poor feeding or vomiting
- Breathing problems or seizures
- Bulging or tense fontanelle (soft spot)
- Unconsciousness or altered level of consciousness
2. How can healthcare professionals differentiate AHT from accidental head injuries?
Healthcare professionals can differentiate AHT from accidental head injuries by closely analyzing the child’s clinical presentation, the caregiver’s explanation of the injury, and the presence of injuries in other parts of the body. AHT often involves multiple injuries that are inconsistent with the caregiver’s explanation, such as retinal hemorrhages, rib fractures, or bruises on the face or head.
3. What are the long-term consequences of AHT?
The long-term consequences of AHT can vary depending on the severity of the initial injury. Some children may experience permanent physical or cognitive disabilities, including intellectual impairment, developmental delays, seizures, or paralysis. Others may have behavioral or emotional problems, such as aggression, hyperactivity, or difficulty with social interactions. Early intervention and appropriate support services are crucial in optimizing the child’s outcome.
4. What is the role of healthcare professionals in preventing and addressing AHT?
Healthcare professionals play a vital role in preventing and addressing AHT. They can educate parents, caregivers, and the community about the dangers of shaking infants and provide strategies for safe infant care. They can also assess and monitor children for signs of abuse, report any suspected cases to the appropriate authorities, and ensure that affected children receive the necessary medical and psychosocial support.
5. How can healthcare professionals support families affected by AHT?
Healthcare professionals can support families affected by AHT by providing compassionate and non-judgmental care. They can offer resources and referrals to appropriate support services, such as counseling, parent support groups, or early intervention programs. They can also help families navigate the legal and child protection systems and advocate for the child’s well-being.
What is pediatric abusive head trauma?
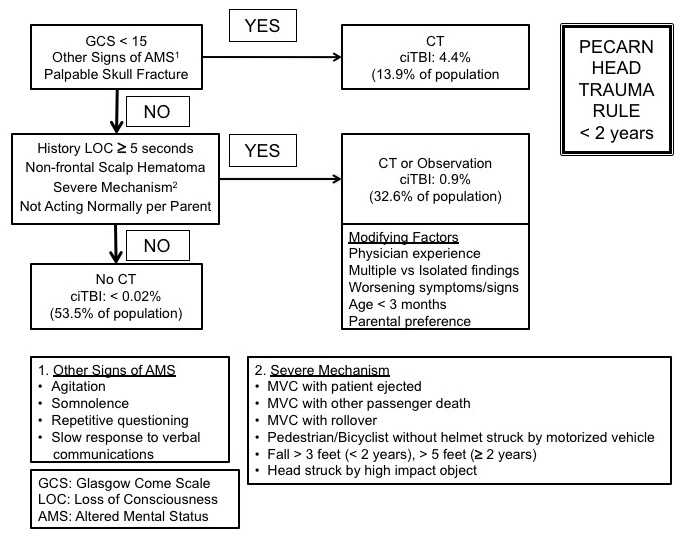
Pediatric abusive head trauma (PAHT) is a severe form of child abuse that involves intentional head injuries inflicted on infants or young children. Also known as shaken baby syndrome or abusive head injury, PAHT can result in devastating and life-threatening consequences for the child.
The most common cause of PAHT is violent shaking of the baby or young child, often by a caregiver who becomes frustrated or overwhelmed with their crying. The shaking motion causes the child’s brain to move rapidly back and forth within the skull, leading to bleeding, swelling, and damage to the brain tissues. In some cases, direct blows to the head or impact with a hard surface may also contribute to PAHT.
PAHT can have long-lasting effects on the child’s development, physical health, and cognitive abilities. The severity of the effects depends on the extent of the brain injury and the promptness of medical intervention. Some potential consequences of PAHT include cognitive impairments, motor deficits, seizures, hearing or vision loss, and even death.
Recognizing the signs of PAHT is crucial for early identification and intervention. Common symptoms may include irritability, lethargy, poor feeding, vomiting, seizures, or changes in behavior. It is essential for healthcare professionals, caregivers, and the community to be educated on the dangers of PAHT and work together to prevent and address cases of abuse.
Signs and Symptoms of Pediatric Abusive Head Trauma
Pediatric abusive head trauma, also known as shaken baby syndrome, is a serious condition that occurs when a baby or young child is violently shaken, causing injury to the brain. It is important to recognize the signs and symptoms of pediatric abusive head trauma in order to seek immediate medical attention and protect the child from further harm.
Some of the common signs and symptoms of pediatric abusive head trauma include:
- Changes in behavior: Children may exhibit sudden changes in their behavior, such as irritability, excessive crying, or difficulty sleeping. They may also become withdrawn or lose interest in activities they once enjoyed.
- Physical indicators: There may be visible signs of injury, such as bruises, swelling, or bleeding in the head or neck area. Other physical indicators include seizures, vomiting, or difficulty breathing.
- Changes in consciousness: Children with abusive head trauma may experience altered levels of consciousness, ranging from drowsiness to unconsciousness. They may have difficulty waking up or seem disoriented.
- Neurological symptoms: Pediatric abusive head trauma can cause neurological symptoms, such as loss of coordination, muscle weakness, or paralysis. Babies may have difficulty feeding or appear floppy.
If you suspect a child may be a victim of pediatric abusive head trauma, it is crucial to seek immediate medical attention. Prompt diagnosis and treatment can help prevent further damage to the child’s brain and improve their chances of recovery.
How is pediatric abusive head trauma diagnosed?
Pediatric abusive head trauma (PAHT), also known as shaken baby syndrome, is a serious condition that requires prompt diagnosis and intervention to prevent further harm to the child. Diagnosis of PAHT involves a comprehensive evaluation that includes a combination of medical history, physical examination, imaging studies, and laboratory tests.
During the medical history interview, healthcare providers will ask the caregivers about the child’s symptoms, any previous incidents or injuries, and any changes in the child’s behavior or development. This information helps in understanding the context and identifying potential signs of abuse. Caregivers may be hesitant to disclose abuse due to fear or guilt, so it is crucial for healthcare providers to create a safe and non-judgmental environment to encourage open communication.
Physical examination plays a significant role in diagnosing PAHT. Healthcare providers will carefully assess the child’s head and neck for any signs of trauma, such as bruises, swelling, or skull fractures. They will also check for any neurological abnormalities, such as abnormal eye movements, seizures, or changes in consciousness. The presence of retinal hemorrhages, subdural hematomas, or other intracranial injuries strongly suggests abusive head trauma.
In addition to the physical examination, imaging studies such as computed tomography (CT) scans or magnetic resonance imaging (MRI) may be ordered to further evaluate the extent of the brain injury and identify any additional injuries. These imaging studies help in visualizing any fractures, bleeding, or swelling within the brain, which can aid in confirming the diagnosis of PAHT.
Laboratory tests such as blood tests may also be conducted to rule out potential underlying medical conditions that could mimic the symptoms of PAHT. These tests can help identify any infections, metabolic disorders, or clotting abnormalities that may be contributing to the child’s symptoms.
What are the risk factors for pediatric abusive head trauma?
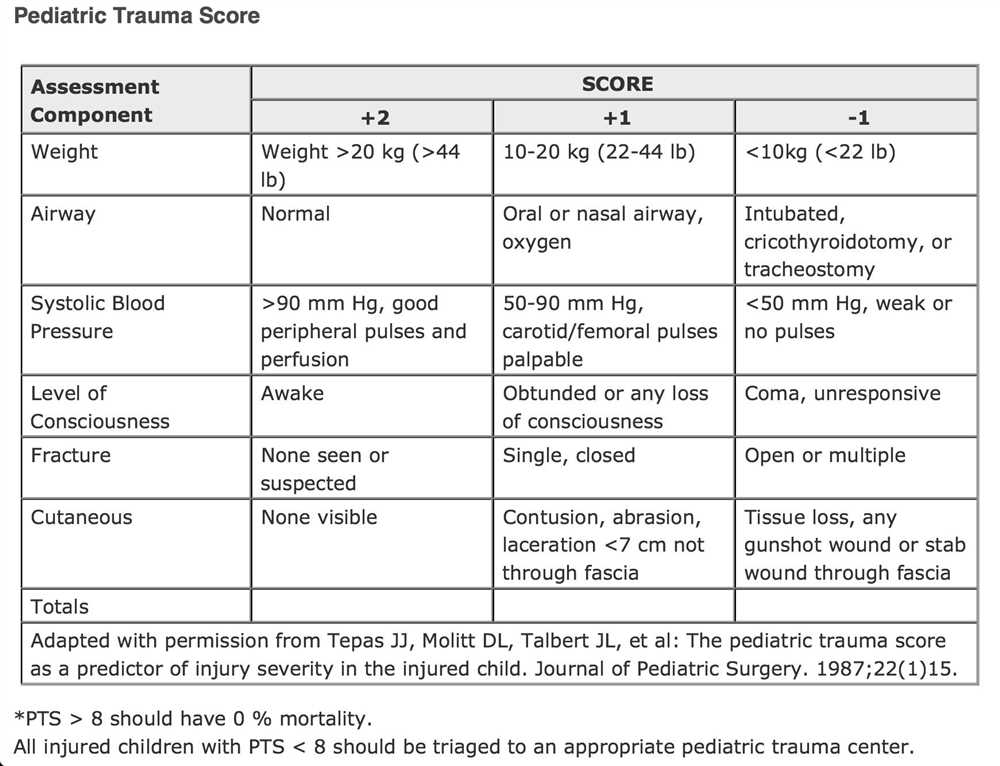
Pediatric abusive head trauma, also known as shaken baby syndrome, is a devastating form of child abuse that can result in serious neurological damage or death. Understanding the risk factors associated with this condition is essential for its prevention and early identification.
Age: Infants aged 0-1 year are at the highest risk for abusive head trauma. Their undeveloped neck muscles and fragile blood vessels make them more susceptible to injury when shaken or subjected to forceful impact.
- Male gender: Studies have found that boys are more likely to be victims of abusive head trauma compared to girls. This may be due to the higher prevalence of aggressive behavior in male caregivers or cultural factors.
- History of abuse: Children who have previously been victims of physical abuse or neglect are at an increased risk of abusive head trauma. It is important to recognize and intervene in cases of abuse to prevent further harm.
- Unexplained injuries: The presence of unexplained injuries, such as bruises, burns, or fractures, in a child should raise suspicion of possible abusive head trauma. These injuries may be inconsistent with the explanation provided by the caregiver.
- Caregiver stress: High levels of caregiver stress, including substance abuse, mental health problems, and financial difficulties, increase the risk of abusive head trauma. These factors may lead to frustration or anger, increasing the likelihood of abusive behavior.
- Isolation: Lack of support systems or social isolation can contribute to high-stress levels in caregivers, making them more susceptible to engaging in abusive behavior.
Recognizing these risk factors and implementing preventive measures and early intervention strategies can help protect children from suffering the devastating consequences of abusive head trauma. Education and awareness about this serious form of child abuse are crucial in detecting and preventing it.
How is pediatric abusive head trauma treated?
Pediatric abusive head trauma (PAHT) requires immediate medical intervention to minimize further damage and provide the best chance for recovery. The treatment approach for PAHT depends on the severity of the injury and the specific symptoms presented by the child.
Medical stabilization: The first step in treating PAHT is to stabilize the child’s condition. This may involve the administration of oxygen, intravenous fluids, and careful monitoring of vital signs. In severe cases, the child may require intubation and mechanical ventilation to ensure adequate oxygenation.
Surgical intervention: In some cases of PAHT, surgical intervention may be necessary to relieve pressure on the brain caused by bleeding or swelling. This may involve the placement of a drain or the removal of blood clots or damaged tissue.
Neurological monitoring and support: Children with PAHT often require close neurological monitoring to assess the extent of brain injury and determine the appropriate treatment course. This may involve regular imaging scans, such as CT or MRI, to monitor changes in the brain. Supportive measures, such as medications to control seizures or maintain blood pressure, may also be necessary.
Rehabilitation and long-term care: Once the child’s condition is stable, a comprehensive rehabilitation program may be initiated to help the child regain lost skills and function. This may involve physical therapy, occupational therapy, speech therapy, and psychological support. Long-term care and ongoing monitoring may also be necessary to address any lingering effects of the trauma.
Prevention and education: It is crucial to also focus on prevention and education to reduce the incidence of pediatric abusive head trauma. Healthcare professionals play an essential role in educating parents and caregivers about the dangers of shaking a baby or causing any intentional harm. By raising awareness and providing support, further cases of PAHT can be prevented.
Can pediatric abusive head trauma be prevented?
Preventing pediatric abusive head trauma is crucial in order to protect infants and young children from this devastating form of abuse. Education and awareness play a vital role in reducing the incidence of this preventable injury.
1. Education for caregivers: Providing education and awareness programs for parents, caregivers, and healthcare professionals can help in identifying the signs and symptoms of abusive head trauma. Teaching caregivers about the dangers of shaking or hitting a baby’s head can ensure they understand the severe consequences of such actions.
2. Safe sleep practices: Promoting safe sleep practices, such as placing infants on their backs to sleep and avoiding co-sleeping, can significantly reduce the risk of abusive head trauma. By creating a safe sleep environment, the likelihood of accidental injury or suffocation can be minimized.
3. Parenting support programs: Implementing parenting support programs can provide caregivers with the necessary skills and resources to effectively manage stress, frustration, and anger. These programs can teach positive discipline techniques and promote healthy coping mechanisms to reduce the likelihood of abusive head trauma.
4. Early intervention: Recognizing and addressing risk factors, such as parental substance abuse, intimate partner violence, or mental health issues, can help prevent pediatric abusive head trauma. Early intervention programs that target these underlying factors can provide support and assistance to families in need.
5. Mandatory reporting: Implementing strong mandatory reporting laws and protocols can ensure that cases of suspected child abuse are promptly reported to the appropriate authorities. Timely intervention and appropriate legal actions can help prevent further episodes of abusive head trauma.
6. Community engagement: Engaging community members, including neighbors, teachers, and healthcare providers, in the prevention of pediatric abusive head trauma is crucial. Creating a supportive and vigilant community environment can help identify and intervene in cases of abuse at an early stage.
7. Research and policy development: Continued research and policy development are essential in the prevention of pediatric abusive head trauma. Understanding the risk factors, identifying effective prevention strategies, and implementing evidence-based policies can make a significant impact in reducing the occurrence of this devastating form of abuse.
In conclusion, pediatric abusive head trauma can be prevented through a combination of education, support programs, early intervention, community engagement, and research. By addressing the underlying causes and promoting a safe and nurturing environment for children, we can work towards eliminating this form of abuse from our society.


